Antiplatelet Medication: What They Are and When to Use Them
If your doctor mentioned an "antiplatelet" drug, you might wonder what that means. In plain terms, these meds stop platelets – the tiny blood cells that help clot – from sticking together. By keeping clots from forming inside arteries, they lower the risk of heart attacks, strokes, and other vascular problems.
Most people hear about aspirin first because it's cheap and widely available. But modern medicine offers several stronger options for people with higher risk or specific conditions. Knowing which one fits your situation can save you a trip to the ER later.
Common Antiplatelet Drugs You’ll See
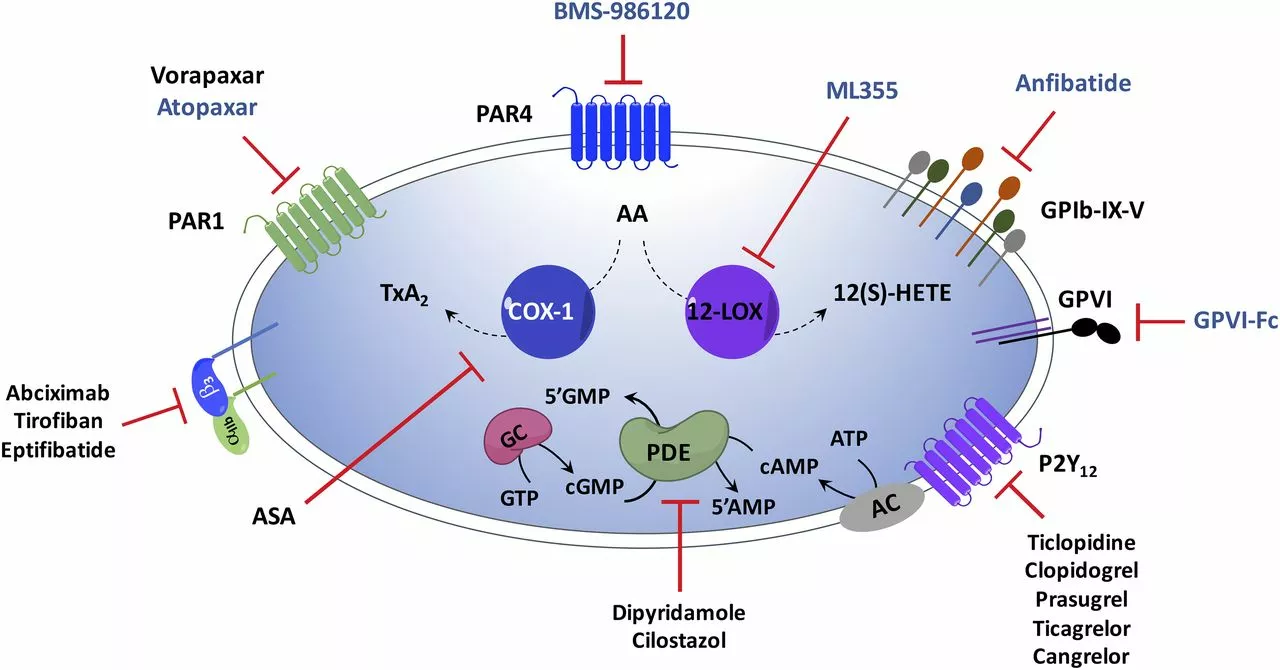
Aspirin (acetylsalicylic acid) – The classic low‑dose (81 mg) tablet is often prescribed after a heart attack or for anyone with a high risk of clotting. It works by irreversibly blocking an enzyme called COX‑1, which reduces a molecule that tells platelets to clump.
Clopidogrel (Plavix) – Popular for people who can’t tolerate aspirin or need extra protection after stent placement. The usual dose is 75 mg once daily. It targets the P2Y12 receptor on platelets, keeping them from activating.
Ticagrelor (Brilinta) – A newer agent that works faster than clopidogrel and doesn’t need metabolic activation. Doctors often pair it with aspirin after acute coronary syndrome. The standard dose is 90 mg twice daily.
Prasugrel (Effient) – Similar to clopidogrel but more potent, used mainly when patients have undergone percutaneous coronary intervention (PCI). Because of its strength, it’s not recommended for people over 75 or with a history of stroke.
When Doctors Recommend Antiplatelets
You’ll typically hear about antiplatelet therapy after:
- A heart attack (myocardial infarction)
- An ischemic stroke or transient ischemic attack (TIA)
- Placement of a coronary stent
- Peripheral artery disease that limits blood flow to legs
- High‑risk cardiovascular profiles (diabetes, smoking, high cholesterol)
The goal is simple: keep the blood flowing smoothly without forming dangerous clots. Your doctor will weigh the benefits against bleeding risk before picking a drug.
Side Effects and Safety Tips
Because antiplatelets thin your blood, the biggest worry is bleeding. Common signs include easy bruising, nosebleeds, or prolonged bleeding from cuts. If you notice black stools, vomiting blood, or unusually heavy menstrual flow, call a doctor right away.
Aspirin can irritate the stomach lining, so taking it with food or using an enteric‑coated version helps. Clopidogrel and ticagrelor rarely cause severe stomach upset but may lead to shortness of breath in some users – report any breathing issues promptly.
Never stop a prescribed antiplatelet without talking to your doctor. Stopping suddenly can trigger the exact clot you’re trying to avoid. If surgery is planned, discuss timing; usually doctors switch you off a few days before the procedure.
Practical Tips for Daily Use
Keep a pillbox and set a daily reminder on your phone – missing even one dose can reduce protection. Store tablets in a cool, dry place away from direct sunlight.
If you take multiple blood‑thinners (like warfarin or a newer anticoagulant), double‑check with your pharmacist to avoid dangerous interactions.
Regular check‑ups matter. Your doctor may order blood tests to ensure the medication is working and not causing hidden bleeding.
Finally, pair medication with lifestyle changes: quit smoking, eat heart‑healthy foods, stay active, and manage stress. Antiplatelet drugs are powerful tools, but they work best when you support them with healthy habits.
Got questions about which antiplatelet fits your health plan? Talk to your healthcare provider – they can tailor the right regimen for you.
Prasugrel vs. Clopidogrel: Which Antiplatelet Medication is Right for You?
In my recent research on antiplatelet medications, I came across two popular options: Prasugrel and Clopidogrel. Both medications are designed to prevent blood clots and reduce the risk of heart attacks or strokes, but they work in slightly different ways. While Prasugrel is known for its faster onset of action and stronger platelet inhibition, Clopidogrel has been around longer and is generally more affordable. Ultimately, the best choice for you will depend on your individual health needs and your doctor's recommendation. It's essential to have a conversation with your healthcare provider to determine which antiplatelet medication suits your situation best.
More